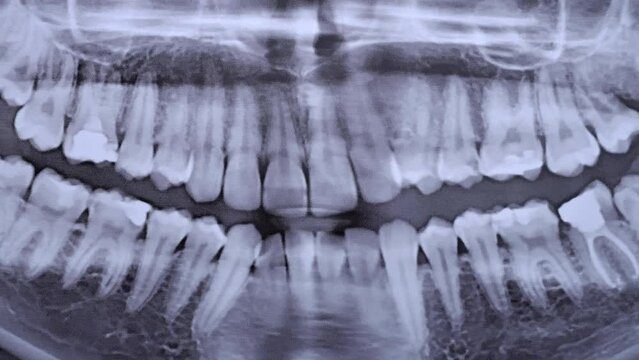
Dental implants revolutionize oral rehabilitation, providing patients with durable, natural-feeling replacements for missing teeth. Successful implant placement relies on several key factors, but bone density consistently proves the most critical determinant. Understanding bone density, assessing it accurately, and implementing strategies to optimize it before implant surgery significantly improves outcomes and patient satisfaction.
Understanding Bone Density
Bone density refers to the amount of bone mineral content present in a given volume of bone. Strong, dense bone supports dental implants, ensuring stability and longevity. Weak or porous bone, in contrast, increases the risk of implant failure and complications. Bone density differs by location in the jaw: the anterior mandible typically has higher density, while the posterior maxilla tends to have softer, less dense bone.
Bone Density and Its Impact on Implant Success
Dental implants achieve success through osseointegration, the process by which the implant fuses with surrounding bone. Higher bone density enhances osseointegration, providing the implant with robust anchorage. Lower density reduces initial stability and delays healing, potentially causing micro-movements that compromise integration. Clinicians observe clear correlations between bone density and implant survival rates, with dense bone consistently supporting longer-lasting results.
For a detailed explanation of how dental implants work and why bone density matters, see Dental Implants Work.
Factors Affecting Bone Density in the Jaw
Several systemic and local factors influence jawbone density. Understanding these factors allows dentists to predict challenges and plan interventions.
Age
As people age, bone naturally loses density. Postmenopausal women experience accelerated bone loss due to declining estrogen levels. Age-related bone changes reduce the jaw’s capacity to support implants, necessitating careful assessment and, in some cases, preparatory procedures such as bone grafting.
Systemic Health
Conditions such as osteoporosis, diabetes, and chronic inflammatory diseases directly impact bone quality. Osteoporosis, in particular, reduces bone mass, weakening the jawbone. Patients with diabetes may experience delayed bone healing, affecting osseointegration. Clinicians must evaluate medical history thoroughly and collaborate with patients’ physicians to ensure safe implant placement.
Lifestyle Factors
Lifestyle choices strongly influence bone density. Smoking decreases blood flow to bone, reducing healing capacity. Poor nutrition, particularly inadequate calcium and vitamin D intake, weakens bone structure. Sedentary lifestyles contribute to bone loss over time. By addressing these factors preoperatively, clinicians can optimize conditions for implant success.
Tooth Loss Duration
The longer a tooth remains missing, the more the surrounding bone resorbs. Immediate implant placement after extraction preserves bone, while delayed placement may require augmentation. Bone resorption patterns vary, but significant volume loss in the posterior maxilla is common, often necessitating grafts or sinus lifts. Learn why timely dental implants can transform outcomes at Lost a Tooth? This Might Be the Best Decision You’ll Ever Make.
Assessing Bone Density for Dental Implants
Accurate evaluation of bone density ensures precise implant planning. Dentists employ several tools and techniques to measure and visualize bone quality and quantity.
Clinical Examination
Initial assessment begins with a thorough clinical examination. Dentists palpate the jawbone to estimate firmness and visually evaluate ridge morphology. While useful, clinical assessment alone cannot reliably quantify density, making imaging essential.
Radiographic Analysis
Advanced imaging provides objective insight into bone density. Cone beam computed tomography (CBCT) scans offer three-dimensional views of the jaw, revealing volume, thickness, and density distribution. Panoramic X-rays provide broader context but lack the detail needed for precise planning. Radiographic analysis guides implant size, placement angle, and the need for augmentation procedures.
Bone Quality Classification
Clinicians often categorize bone into types based on density. One common classification is:
- Type I: Dense cortical bone, high stability, excellent implant support.
- Type II: Thick cortical bone with dense trabecular bone, favorable for osseointegration.
- Type III: Thin cortical bone with low-density trabecular bone, moderate risk of complications.
- Type IV: Very soft bone, high risk for implant failure, may require grafting or special implant techniques.
To explore the types of dental implants suitable for different bone densities, visit Types of Dental Implants.
Planning Implants Based on Bone Density
Bone density directly influences surgical strategy, implant selection, and loading protocols. Clinicians tailor procedures to match the bone’s capacity to support implants safely.
Implant Selection
Denser bone allows the use of standard-length and standard-diameter implants, while softer bone may require wider or longer implants to distribute forces more effectively. Surface treatments, such as roughening or coating, improve osseointegration in low-density bone. Selecting the right implant reduces the risk of early failure and enhances long-term stability. For expert guidance on dental implant options, check Best Dental Implant Options for Missing Teeth.
Preoperative Bone Augmentation
When bone density or volume proves insufficient, augmentation becomes necessary. Bone grafting introduces autogenous, allogenic, or synthetic bone material to reinforce the jaw. Sinus lifts elevate the sinus floor to allow implant placement in the posterior maxilla. Ridge expansion techniques widen narrow alveolar ridges. These interventions create a strong foundation, ensuring implants integrate properly. Learn more about the dental implant surgery process at Dental Implant Surgery.
Surgical Technique Adaptations
Surgeons modify drilling speed, depth, and sequence depending on bone density. Denser bone requires slower drilling to avoid heat damage, while softer bone may benefit from under-preparation to enhance primary stability. Clinicians carefully balance these variables to maximize implant success rates.
Loading Protocols
Bone density determines when clinicians load implants with crowns or bridges. High-density bone tolerates immediate loading, providing quicker restoration. Softer bone often necessitates delayed loading to allow gradual osseointegration. Following appropriate protocols prevents implant mobility and failure.
Optimizing Bone Health Before Implants
Proactive strategies can improve bone quality and support implant success. Dentists advise lifestyle changes, dietary improvements, and medical interventions when necessary.
Nutrition and Supplements
Calcium and vitamin D are essential for bone metabolism. Patients may require supplementation to achieve optimal levels. Protein intake supports bone matrix formation, while other micronutrients such as magnesium, vitamin K2, and phosphorus enhance mineralization. Nutritional optimization strengthens bone before surgery and supports healing afterward.
Lifestyle Modifications
Smoking cessation, weight-bearing exercise, and avoidance of excessive alcohol promote bone density. Consistent physical activity stimulates bone remodeling, increasing strength. Patients who adopt these habits improve their implant prognosis significantly.
Medical Management
For patients with osteoporosis or systemic bone conditions, physicians may prescribe medications such as bisphosphonates or selective estrogen receptor modulators to improve bone density. Clinicians coordinate with medical providers to ensure these therapies complement implant treatment safely.
Conclusion
Bone density remains a cornerstone of successful dental implant planning. Clinicians who understand its importance, assess it accurately, and optimize conditions before surgery achieve higher success rates, faster healing, and better patient outcomes. Bone density affects implant choice, surgical technique, loading timing, and the need for augmentation procedures. By prioritizing bone health, dentists ensure dental implants provide durable, functional, and aesthetically pleasing results for patients. Failing to consider bone density risks implant failure, extended treatment times, and additional procedures.
Patients benefit when dental teams take a proactive, comprehensive approach to bone evaluation and enhancement. Through thorough assessment, careful planning, and evidence-based strategies, clinicians transform potential challenges into predictable, successful outcomes. Ultimately, recognizing the critical role of bone density empowers both dentists and patients to make informed decisions that maximize the long-term benefits of dental implant therapy.
Investing in bone health before implants delivers lasting value. By addressing bone density upfront, dentists create a strong foundation for restoration, reduce complications, and support patient satisfaction. Every implant achieves its full potential when the underlying bone possesses the strength and integrity required to sustain it. Book a consultation today at Want Teeth Appointment to begin your dental implant journey.
© 2026 Dental Implant Insights. All rights reserved.