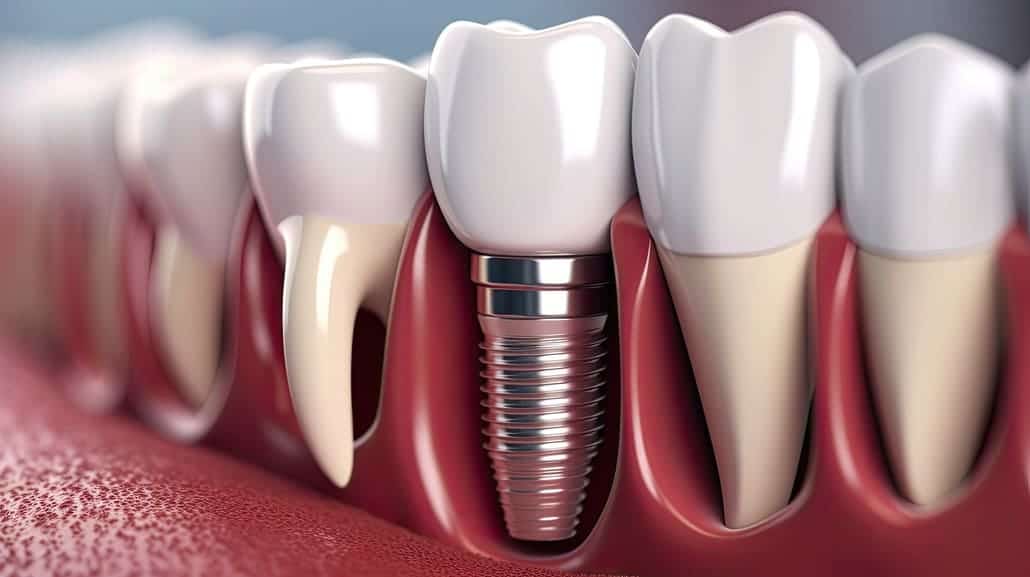
Dental implants have revolutionized modern dentistry, offering patients a durable and natural-feeling solution for tooth loss. While many patients assume that implants always succeed, outcomes vary depending on numerous factors, including surgical technique, patient health, and post-operative care. This article provides an in-depth, evidence-based look at dental implant success rates, key influencing factors, and strategies to maximize outcomes.
Understanding Dental Implant Success
Dental implant success does not solely depend on the implant staying in place. Experts evaluate success using multiple criteria, including functional stability, absence of pain, healthy surrounding bone, and aesthetic outcomes. According to clinical studies, modern dental implants boast success rates between 90% and 98% over a ten-year period, making them a reliable solution for tooth replacement.
Defining Success and Failure
Dental implant failure occurs when the implant cannot integrate with the jawbone or causes persistent discomfort. Early failures typically happen within the first year and often result from surgical errors, infection, or poor bone quality. Late failures occur years after placement and usually relate to systemic health issues, peri-implantitis, or excessive mechanical stress. For a detailed overview of how implants work, visit How Dental Implants Work.
Factors Influencing Implant Success Rates
Implant success depends on a combination of biological, technical, and patient-related factors. By understanding these variables, clinicians can better predict outcomes and customize treatment plans for individual patients.
1. Bone Quality and Quantity
The jawbone must provide adequate support for implant stability. Dense bone in the anterior mandible generally offers higher success rates than softer posterior maxillary bone. Clinicians often perform bone grafts or sinus lifts to enhance bone volume and improve outcomes in cases of insufficiency.
2. Surgical Technique
Experienced surgeons achieve higher success rates through meticulous planning and precise execution. Factors such as proper implant angulation, correct drilling protocols, and atraumatic tissue handling significantly influence osseointegration. Using guided surgery techniques further improves accuracy and predictability.
3. Implant Design and Material
Implant surface technology, diameter, length, and material impact success. Titanium implants with roughened surfaces integrate more effectively with bone than smooth implants. Recent innovations, including zirconia implants, offer high biocompatibility and aesthetic advantages, although long-term data remains limited. To explore the types of implants available, see Types of Dental Implants.
4. Patient Health and Lifestyle
Systemic conditions such as diabetes, osteoporosis, and immune disorders affect bone healing and implant integration. Smoking reduces blood flow to the jaw and significantly increases the risk of implant failure. Optimizing systemic health and addressing lifestyle factors before surgery enhances outcomes.
5. Oral Hygiene and Maintenance
Patients who maintain excellent oral hygiene enjoy better implant longevity. Regular dental check-ups, professional cleanings, and proper brushing and flossing reduce the risk of peri-implant diseases, which remain a leading cause of long-term implant failure. Learn more about professional dental implant services at WantTeeth Dental Implants.
Short-Term vs Long-Term Success Rates
Dental implant success differs in the short-term versus long-term. Clinicians observe early osseointegration success within 3–6 months after surgery. Long-term success involves maintaining bone levels, tissue health, and functional stability over 10–20 years. Studies indicate that early success rates are typically above 95%, while long-term success averages 90–95%, demonstrating implants’ durability when properly managed.
Complications Affecting Success
Even with optimal planning, complications can reduce success rates. Clinicians categorize complications as biological or mechanical, each requiring specific interventions.
Biological Complications
- Peri-implantitis: Inflammation around the implant can lead to bone loss and failure if untreated.
- Infections: Post-surgical infections may compromise osseointegration.
- Poor bone healing: Conditions like osteoporosis or smoking hinder bone regeneration around the implant.
Mechanical Complications
- Implant fracture: Excessive occlusal forces or faulty implant design may cause breakage.
- Prosthetic loosening: Crowns or abutments can loosen if occlusal forces exceed implant tolerance.
- Wear and tear: Implants can experience micro-movements leading to gradual bone resorption over time.
Evidence from Clinical Studies
Researchers have conducted numerous longitudinal studies to evaluate dental implant outcomes. A meta-analysis of over 15,000 implants found cumulative success rates of 92% after ten years. Another study reported that patients with healthy bone and no systemic risk factors achieved success rates above 95%, reinforcing the importance of patient selection and proper planning.
Strategies to Maximize Success
Clinicians can adopt several strategies to improve implant outcomes and patient satisfaction.
1. Comprehensive Treatment Planning
Thorough assessment of bone quality, systemic health, and aesthetic expectations allows clinicians to select the ideal implant type, size, and surgical approach. Learn more about the clinic and its team at About WantTeeth.
2. Pre-Surgical Optimization
Patients benefit from addressing modifiable risk factors before surgery. Smoking cessation, managing diabetes, and improving oral hygiene enhance healing potential.
3. Advanced Surgical Techniques
Computer-guided implant placement improves accuracy and reduces surgical trauma. Using minimally invasive techniques minimizes post-operative complications and speeds recovery.
4. Post-Operative Care and Maintenance
Regular follow-ups, professional cleanings, and patient education on hygiene practices prevent peri-implant diseases. Clinicians recommend radiographic monitoring to detect early bone loss. When ready to schedule a consultation, patients can book online via WantTeeth Appointment.
Patient Considerations and Expectations
Successful outcomes also depend on managing patient expectations. Patients should understand that implants require lifelong maintenance and occasional adjustments. Educating patients about potential risks, healing timelines, and the importance of follow-up care enhances satisfaction and long-term results.
Future Directions in Implantology
Innovations in implant materials, surface treatments, and digital dentistry promise to further improve success rates. Research in biomimetic coatings, 3D-printed implants, and personalized surgical guides enhances predictability and reduces complications. As evidence accumulates, clinicians can implement more precise, patient-specific approaches to maximize long-term success.
Conclusion
Dental implants provide a reliable and highly successful solution for tooth replacement when clinicians and patients work together to optimize outcomes. Success rates approach 95% over ten years when proper planning, surgical expertise, patient health, and diligent post-operative care are prioritized. By understanding the factors influencing success and adhering to evidence-based practices, both clinicians and patients can achieve durable, functional, and aesthetically satisfying results.
Dental implant therapy continues to evolve, offering new tools and techniques to improve outcomes. Patients benefit most when clinicians combine technical expertise with individualized care and continuous follow-up. With the right approach, dental implants represent a long-term, predictable solution that restores oral health and quality of life.
© 2026 Dental Insights. All Rights Reserved.